What is a pressure sore (decubitus ulcer)?
A pressure sore consists of skin or tissue damage that occurs when there is a decrease in blood circulation due to pressure in a specific area.
Initially slight redness on the affected area can be noticed (the first sign of tissue damage). The tissue underneath it perishes due to poor blood supply. Various skin layers, muscles and bones can be affected.
Every patient, who stays immobile due to chronic illness or during post–operative period, is exposed to high risk of developing pressure ulcers.
In the patient’s care program during his hospital stay as well as at home, the patient and his family are informed about the risk factors and preventive measures, they have to take to avoid pressure ulcers.
If a pressure ulcer is already formed, wound management combined with the application of modern wound dressings and pressure reliving devices is necessary.
Risk factors:
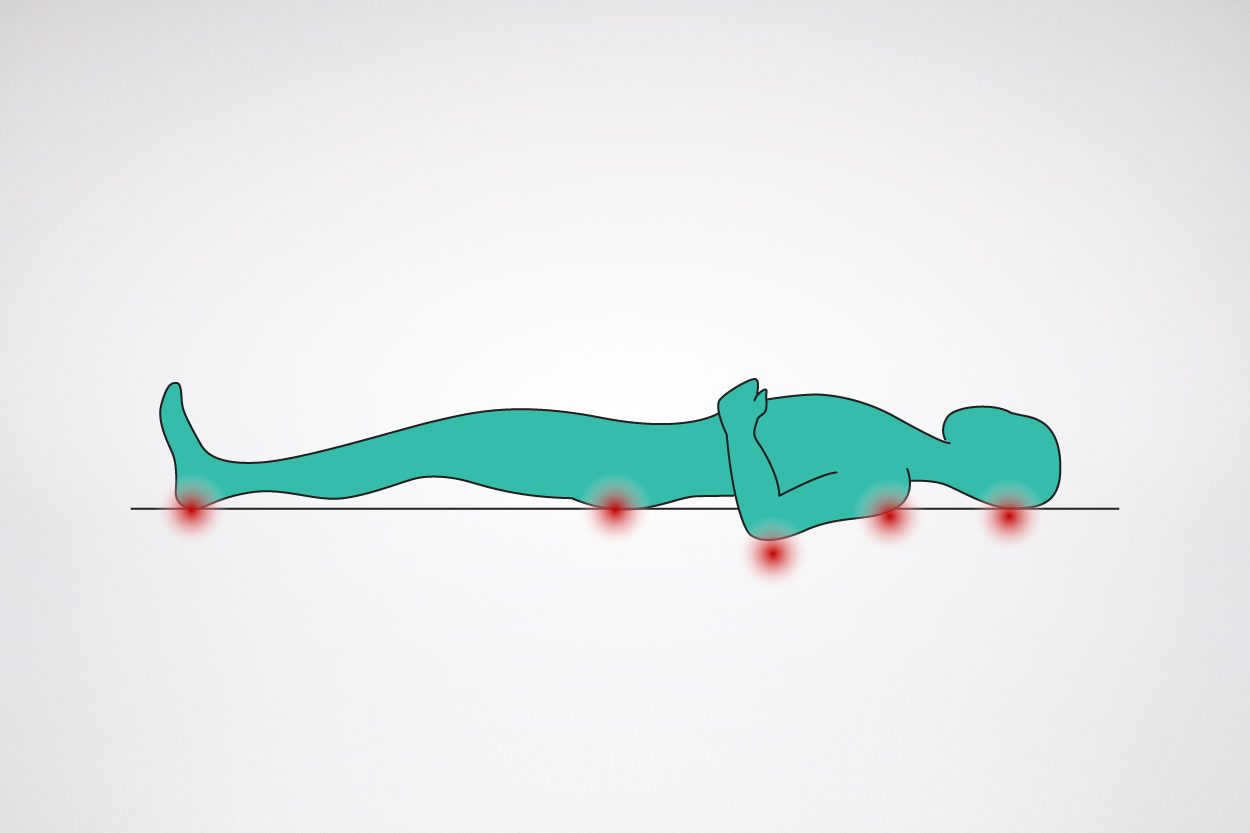
The most important cause of tissue damage leading to pressure ulcers is the buildup of pressure. Tissue damage is proportional to pressure intensity and the duration of capillary compression.
Other factors contributing to the risk of developing pressure ulcers:
- Ageing
- Smoking
- Skin status: elasticity, edema, dryness
- Tissue hypoxia, caused by underlying disease
- Nutritional anomalies (being overweight or underweight)
- Immunological anomalies
- Neurological disorders
- Altered level of consciousness
- Incontinence
- Medications
- Decreased mobility, caused by pain, tiredness or stress
- Hygiene deficit
- Lack of knowledge of potential damage
Preventive measures:
Changing patients' position:
One of the simplest and most effective measures is changing the patient’s position frequently.
- If the patient is unable to change position himself, caregivers and healthcare professionals should assist him.
- People who are confined to bed need to change their position at least once every two hours.
- The person in a wheelchair should change position at least every 15 to 30 minutes.
If a pressure ulcer is already formed, it is important to avoid putting additional pressure on it, either by regular repositioning or by using pressure off-loading devices. This will give the wound the best chance of healing.
Follow a healthy and balanced diet:
A healthy and balanced diet with an adequate amount of protein, vitamins and minerals helps prevent skin damage, it will help wounds heal faster. If necessary, the patient may be referred to a dietitian who will establish a dietary plan for him.
Take care of the skin:
It is important to inspect the areas of skin at risk daily. You can use a mirror to check the parts of your body that are difficult to see, such as your buttocks and heels. If you notice any change, skin discoloration (permanent redness, brown color) you should contact your healthcare professional, GP or community nurse if you are at home, or one of your nurses if you are in a hospital or nursing home.
Skin at risk:
The skin discoloration may indicate stage 1 pressure ulcer, which should be treated correctly before developing skin damage, which may be painful and often takes a long time to heal.