Reduce hypos and lipos
Many patients have areas of lipohypertrophy (lipo) but they are often unaware of them or mistake them for muscle development. They might even prefer to inject into lipos as the areas are less sensitive and pain on injection is reduced. However, the link between lipos and hypos (hypoglycemic episodes) has been the topic of many studies. It is clear that improving injection technique and reducing lipos will reduce hypos.
Why are lipos risky for your patients?
- 2 out of 3 patients with diabetes have areas of lipohypertrophy caused by poor injection technique such as reusing needles or not rotating their injection sites correctly*
- 98% of patients with areas of lipohypertrophy do not rotate injection sites correctly*
- 49% of patients with areas of lipohypertrophy have unpredictable glucose levels which could lead to hypos*
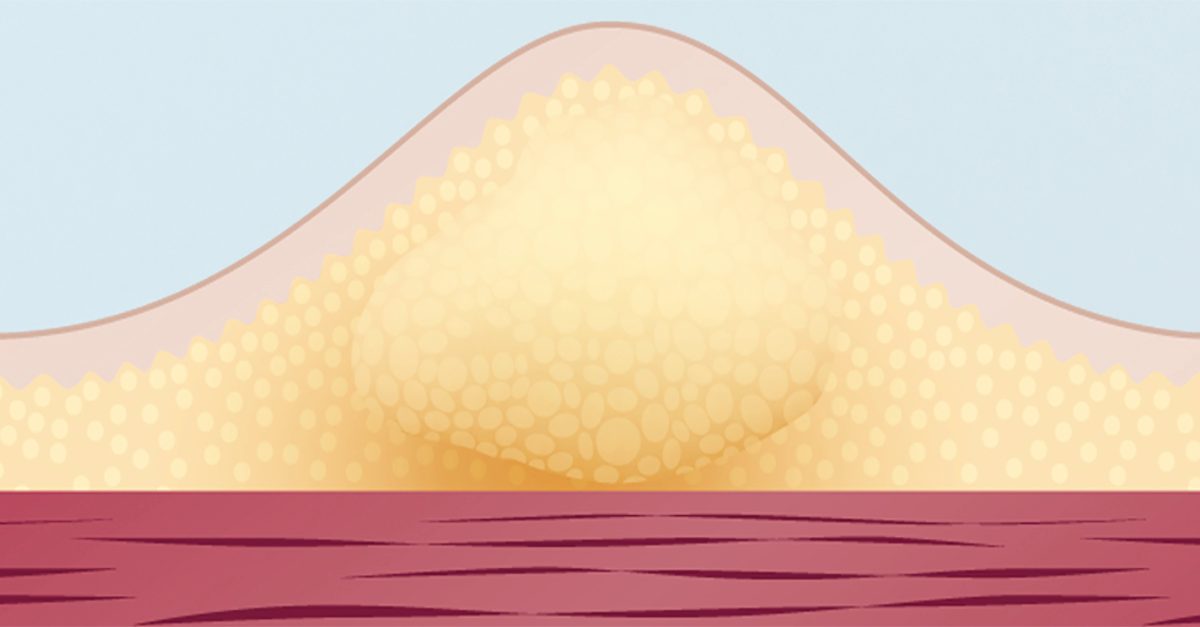
What are lipos?
Lipos or Lipohypertrophies as they are more formally known as are thickened, rubbery areas of fatty tissue caused by:
- Incorrect injection site rotation technique, leading to repeated injections into the same site
- Repeated use of a single use pen needle, leading to needles which have become blunt
- Prolonged use of injectable therapies
Why do lipos cause hypos (hypoglycaemia)?
- The absorption rate when injecting into areas of lipos is unpredictable
- Absorption unpredictability when injecting medication can lead to vast glycaemic variation which can cause unexpected hypos
Omnican® fine pen needles
As hypos can be the result of poor injection technique and as we are a manufacturer of the high quality Omnican® fine 32G pen needles, we provide a comprehensive range of injection technique literature for health care professionals and their patients. With the aim to improve injection technique and reduce hypos.
Take a look at the educational literature we offer, if you like them, please order via sample request form below.
Injection Technique Folder & Site Rotation Templates
Trend: Injection Technique Matters (For Health Care Professionals)
Trend: Injection Technique Matters Toolkit (For Patients)
„We Protect and Improve the Health of People around the World “
Sources
*Blanco M. et al. Prevalence and risk factors of lipohypertrophy in insulin-injecting patients with diabetes. Diabetes & Metabolism 39 (2013) 445–453