The problem - Reduced dressing changes
Reduced patient contact? Patients going longer between dressing changes?
According to recent evidence, due to Covid-19, 82% of clinicians have seen a decrease in patient contact and, 60% patients stated their dressing change frequency had dropped dramatically.1
How are your handling the challenge posed by decreased patient contact?
Concerned about the negative effects of leaving dressings on for longer?
According to UK clinicians, prior to Covid-19, dressing change frequency was every 2-3 days with exudate levels, signs of infection and patient comfort sited as reasons to initiate a dressing change.2
What are you going to do differently?
The solution - Cleanse | Debride | Prevent
The answer: Cleanse | Debride | Prevent
Cleanse, Debride and Prevent are three key treatment outcomes. Our three step solution will help to you take wound bed preparation seriously, give you more confidence when you’re away from your patients, and help to heal wounds 4 weeks faster.3
For information on our wound cleaning and debridement focused pages, follow the links below.
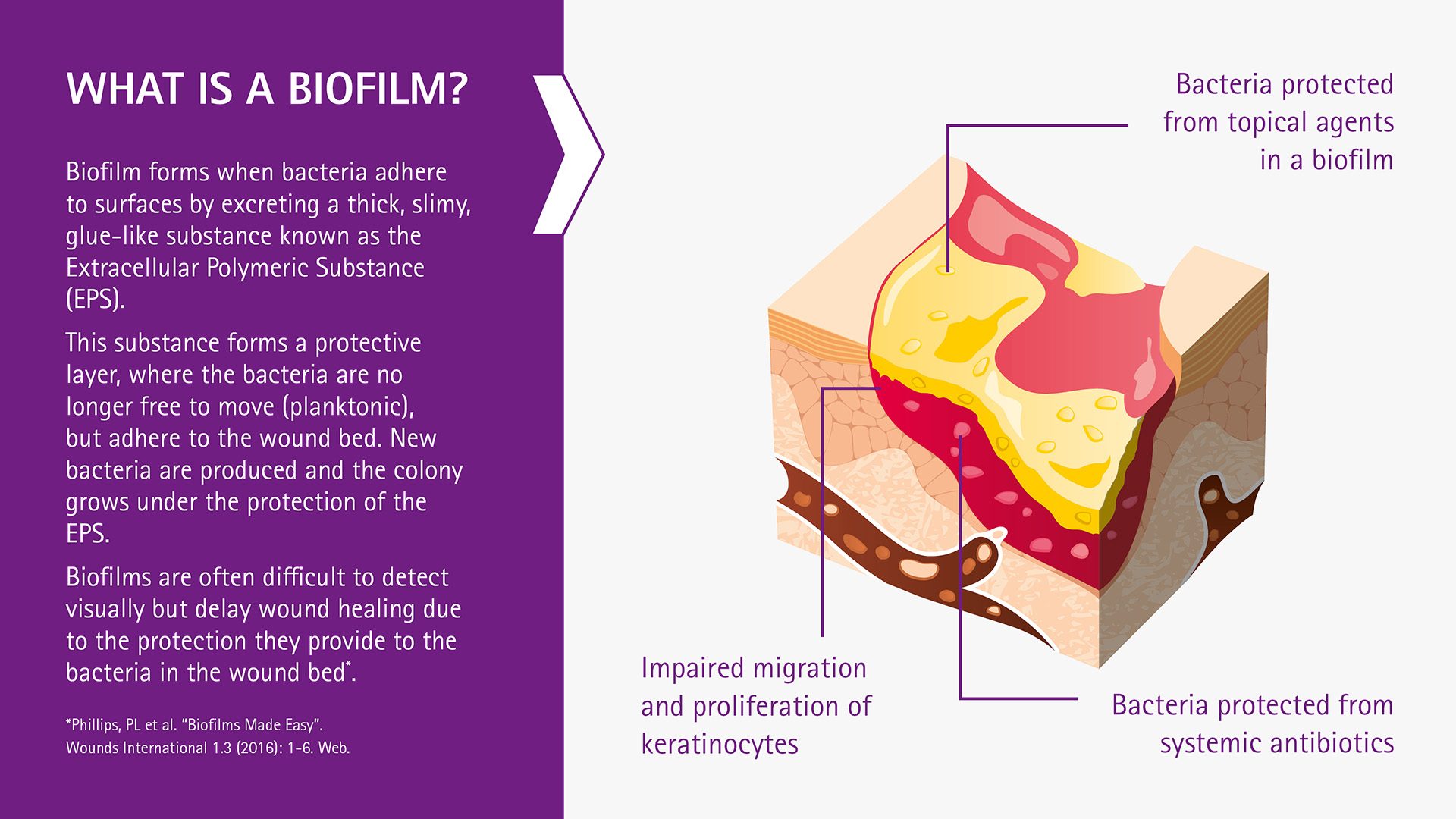
Why is 'prevent' so important?
You may cleanse or debride already, but why is 'prevent' so important?
Even after cleansing and debridement, biofilm can reform within 6hrs, with mature wound biofilm forming in 2-4 days – with fewer dressing changes it’s likely that most of the wounds seen right now present with a mature biofilm at every dressing change.
Biofilms increase slough and exudate, can be a source of infection and contribute to delayed healing.4
You can read more about biofilms on our dedicated biofilm page.
What do high levels of exudate and inflammation mean to you and your patients?
Clinical evidence
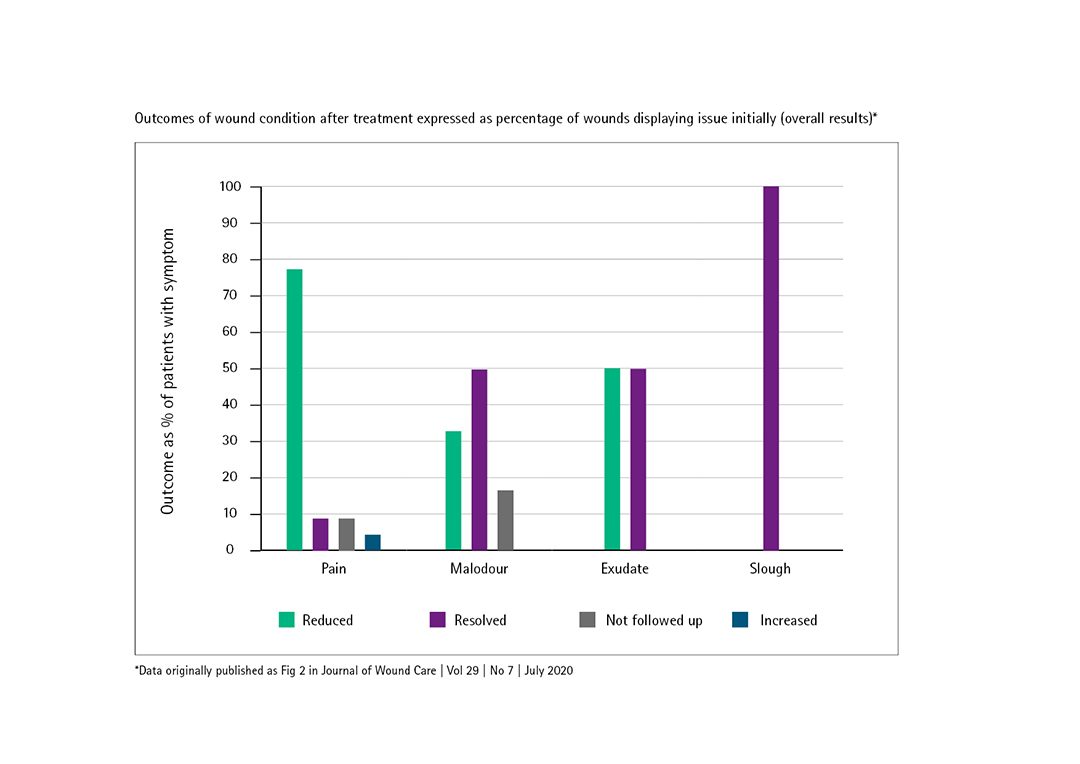
Reduced dressing change frequency and faster healing.
Our recent Journal of Woundcare article demonstrates that by using a combination of Prontosan Gel X to protect the wound bed alongside using Prontosan Solution to initially cleanse the wound bed, levels of slough, exudate and malodour were improved or resolved.
Importantly, dressing change frequency was able to be reduced by 55% .5
Prontosan® Gel X info
Protect your wounds with Prontosan® Gel X
Prontosan Gel X can be left in place until the next dressing change to continue wound cleansing and help prevent biofilm reformation.
"Use Prontosan® as a combined system"
“My main objectives in leg ulcer care are to free wounds from infection or biofilm, manage exudate and debride any slough or necrotic tissue from the wound bed.”
"I have found that using all three products in combination works particularly well… Together, all three stop biofilm reforming, reduce healing time and help to prevent wound infection“
Read more about Practice Nurse, Katie Bennett’s experience using the Prontosan range of products for wound bed preparation in this Practical Patient Care article.
Helping your patients
How can you help your patients right now?
We know that dressing change frequency has reduced during the Covid-19 pandemic. We know that more patients are having to self-care at times. We know that you are under pressure and new product solutions may not be top of your to do list.
However, we know that Prontosan Gel X can help you and your patients right now by helping to reduce dressing change frequency, helping to disrupt biofilm and in healing wounds faster.
Complete the contact form below and we will be in touch with materials to support you.
Further information
Contact us
Ordering info
How do you order Prontosan® Gel X?
Prontosan® Gel X is available on Drug Tariff and can be prescribed in single units or packs of 20.
It is also available via NHS Supply Chain in single units or packs of 20.
Ordering codes for the Prontosan® Gel X and the Prontosan® range are available in the table below.
Order samples
Wound Care Blog
-
Prontosan® Debridement Pad | Before and After
Read MoreThe Prontosan® Debridement Pad is intended to support the soft mechanical debridement of chronic wounds in combination with Prontosan® Wound Irrigation Solution.
-
Award Winners! Integrating a Wound Cleansing Pathway into standard care.
Read MoreThe Doncaster Skin Integrity Team recently received a Bronze JWC award in the Infection and Biofilm category for their work on their local Wound Cleansing Pathway.
-
The role of Prontosan® in a pathway for biofilm based wound care
Read MoreAnita Kilroy-Findley, Clinical Lead Tissue Viability, Leicestershire Partnership NHS Trust, shares her experience of using the Prontosan in a pathway for biofilm based wound care.
References
1. Tinelli, G. & Sica, S. (2020) Wound Care during COVID-19 Pandemic
2. Clinician perspective on time and resource related to dressing changes. Available at https://www.wounds-uk.com/journals/issue/506/article-details/clinician-perspectives-on-time-and-resources-related-to-dressing-changes [accessed Jan 2021]
3. Andriessen AE, Eberlein T. Assessment of a wound cleansing solution in the treatment of problem wounds. Wounds 2008; 20(6):171–175
4. International Wound Infection Institute. Wound infection in clinical practice. Wounds International, 2016
5. Atkin et al, (2020) Wound bed preparation: a case series using polyhexanide and betaine solution and gel—a UK perspective
6. Valenzuela A, Perucho N. Effectiveness of a 0.1% polyhexanide gel. Rev ROL Enf 2008; 31(4):247-252
7. Durante et al. Evaluation of the effectiveness of a polyhexanide and propyl-betaine based gel in the treatment of chronic wounds. Minerva Chir 2014;69:283-92
8. Collier, Hofer. Taking wound cleansing seriously to minimise risk. Wounds UK Vol 13 No 1 2017
9. Moeller et al. Experiences with the use of polyhexanide-containing wound products in the management of chronic wounds – results of a methodical and retrospective analysis of 953 patients. Wound Management May 2008