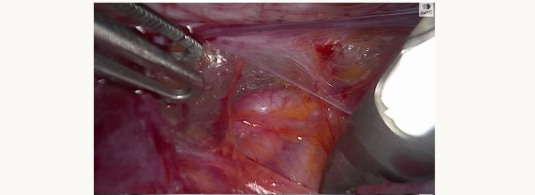
Standard image
You have successfully logged out.
Not registered yet?
Testimonial
Tom Aust, MB ChB, MD, FRCOG
Consultant Obstetrician and Gynaecologist

Tom Aust, MB ChB, MD, FRCOG
I am a Consultant Obstetrician and Gynaecologist in the North West of England and in my hospital I am the lead consultant for the tertiary Endometriosis Service covering referrals from around Merseyside, Cheshire, North Wales and beyond.
I have been a consultant for 13 years, prior to that I trained in the Mersey region and completed a 2-year laparoscopic fellowship in Sydney, Australia. I concentrate on minimally invasive and robotic surgery for deep infiltrating endometriosis and complex laparoscopic hysterectomies.

We have used EinsteinVision® 3D imaging since 2018 and in the last 18 months we have introduced indocyanine green (ICG) into the ureters, bladder, uterus and fallopian tubes. By using fluorescence imaging (FI) the dye makes these structures glow to help their identification during complex laparoscopy.
I find that the 3D image and high definition picture really enhances dissection of tissues, identification of bleeding points and movement of needles and knot-tying when suturing. Prior to using the system, I was not convinced that the 3D image was necessary, having trained exclusively with a 2D flat image. However I now find that if I have to assist general surgical colleagues with their 2D scopes I really miss it. I feel that it brings conventional laparoscopy one step closer to the intuitive feel of robotic surgery.
The use of ICG has helped to improve safety in laparoscopic procedures by making identification of surrounding structures much easier. If endometriosis, fibroids or scarring involve the ureter then the ICG helps me to dissect the disease from it and ensure that the ureter hasn’t been damaged.
Previously the ureter may have required stenting (which is traumatic and causes pain and haematuria) and would require mobilisation and temporary slooping to ensure it is safe. This is still the case if the disease is very close to the ureter. However, the dye means that often if the ureter can be seen to be away from the surgical field then it may not need to be fully dissected out which is less traumatic and quicker.

Standard image
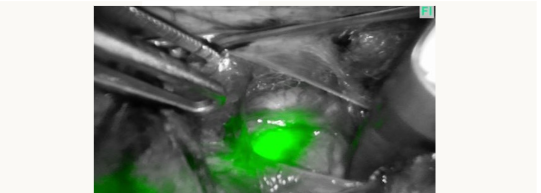
Flurescent image
ICG has been used intravenously since the 1950’s to look at vascularity within the retina and in laparoscopy to help with sentinel lymph node identification and to check the blood flow to the anastomosis after segmental bowel resection.
More recently it has been used within the ureter but has to be instilled directly rather than intravenously as it is hepatically excreted rather than through the renal tract.
The technique for preparation is described below. We have found this dilution works well to show the ureters and allows the extra to be used in other areas such as the bladder/uterus/fallopian tubes.
(NB; this is currently an unlicensed indication for Verdye ICG)
I tend to inject the ICG at the start of the operation by performing a cystoscopy with antibiotic cover, passing a 6Fr ureteric catheter into the first 5 cm of each ureter and injecting 10 ml of solution in a retrograde fashion. The ureteric catheter and cystoscope are then removed.
I tend to use injection of ICG into the ureters in cases where the anatomy of the pelvis is abnormal or very scarred. This is true in operations involving large fibroids in the cervix and pelvic sidewall, deep endometriosis, ovarian cysts extending into the sidewall and uterine and renal tract anomalies where the ureters are particularly at risk. If the ureter is tethered or displaced by fibroids or endometriosis I still have to dissect it free, but being able to identify it easily really helps. In other cases the ICG allows me to see that the ureters are free from where I am working which is very reassuring.
In the past I often had to dissect out the ureter and place a rubber sloop or even consider a ureteric stent but both of these procedures can cause trauma to the ureter. However slooping will only help identifying a portion of the ureter whereas ICG can show the entire length of pelvic ureter (figures 1A and 1B below). Stenting can lead to post-operative pain and haematuria and I don’t find them particularly helpful in identifying the ureter prior to seeing the stent when you transect the ureter!
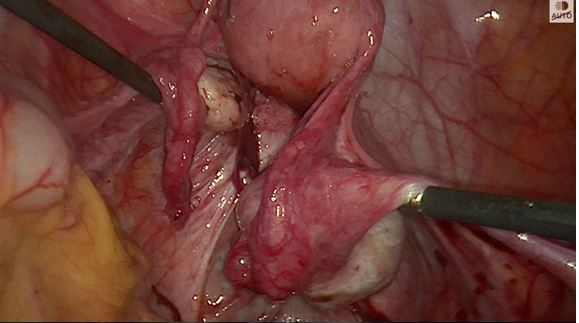
Figure 1A
Path of ureters at the start of endometriosis surgery
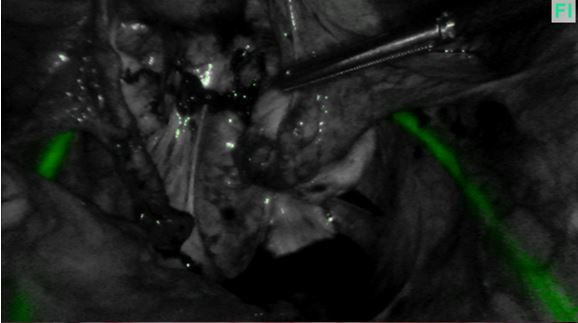
Figure 1B
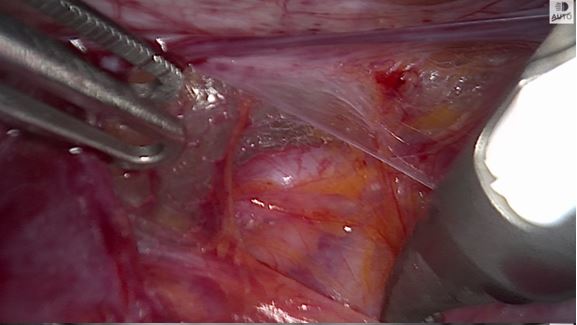
Figure 2A
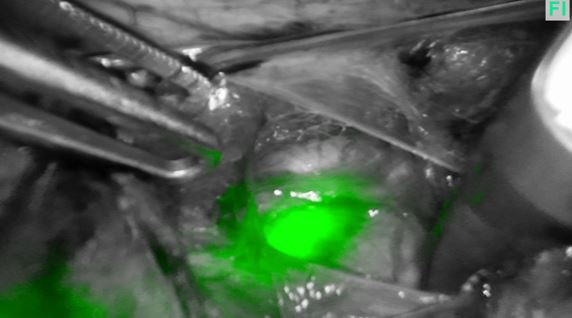
Figure 2B
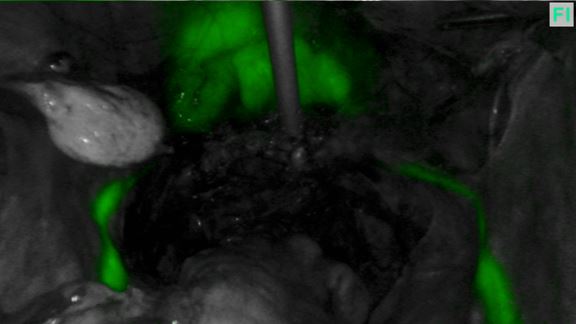
Figure 3
Helping to see the ureter more laterally in the pelvic sidewall can allow safe occlusion of the uterine artery at its source (figures 2A and 2B above) which can be helpful during myomectomies or more complex hysterectomies.
While the ICG dye does gradually pass into the bladder, it stays visible in the ureters for 4 - 5 hours as it seems to stain the urothelium (figure 3 above). We have found that no further intraoperative injections are necessary.
If there is any concern about the integrity of the ureter or any risk of delayed thermal damage then a JJ stent can still be inserted by urology colleagues at the end of the procedure but we find this is rarely required.
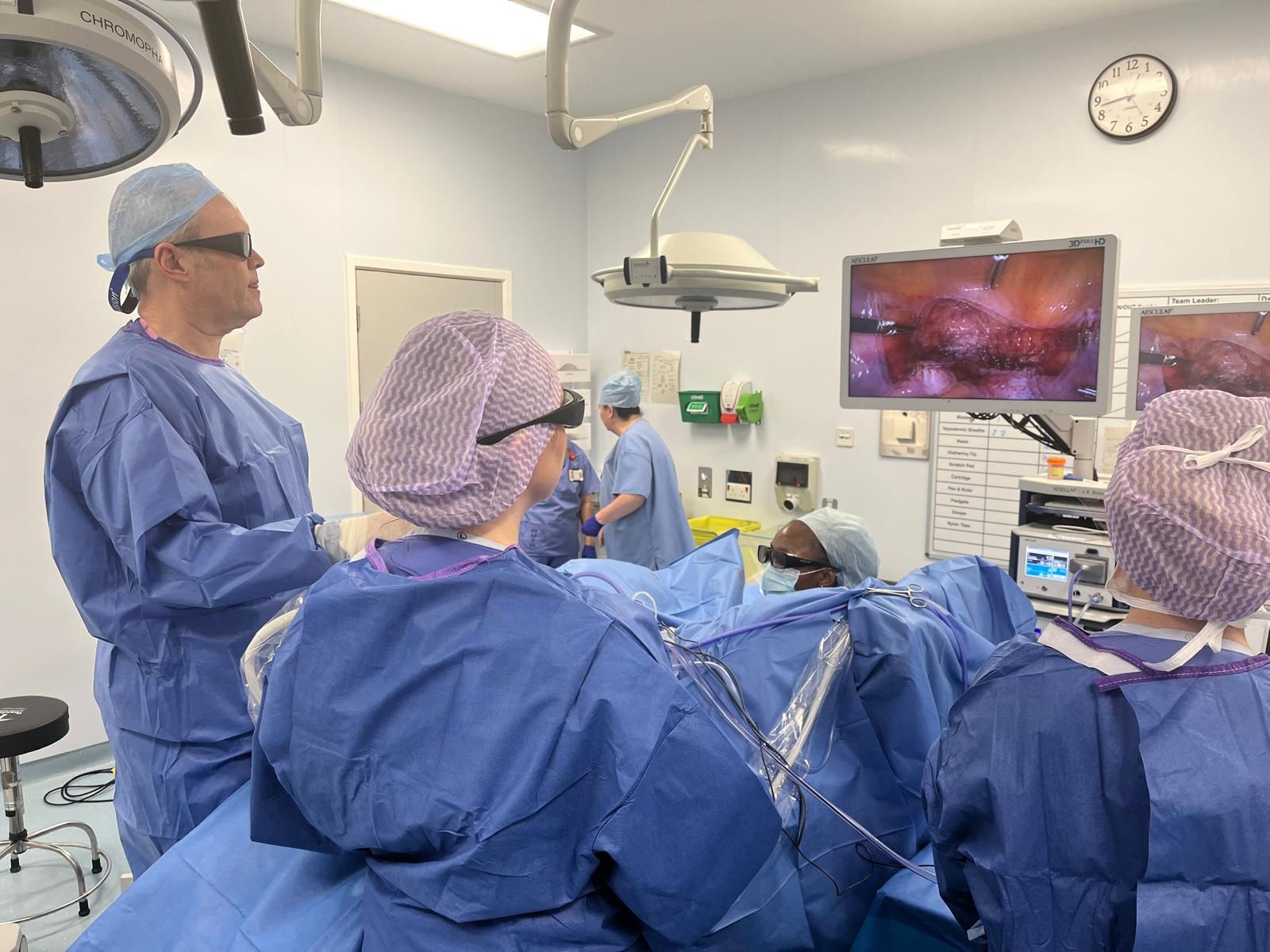
As the system has a single camera/laparoscope unit we have found that fogging of the view has been eliminated. This is because the tip of the scope is heated. If the tip becomes obscured by blood or smoke spatter you can wipe it without fear of scratching the lens as the protective disposable sheath protects it.
My standard entry technique uses Veres needle insufflation then with an optical entry using a 10 mm port with the system set to 2D. I find it isn’t possible to use 3D during entry as the focal point is too close to the scope and you get blurring. I perform a 360-degree inspection and place my secondary ports under vision. I then drop to a working pressure of 12 mmHg, everyone puts on 3D glasses and we switch to 3D for the rest of the operation.
I have found that it is really important to get the HD screens perpendicular to the observers for a clear 3D image, and this may involve platforms/steps when sharing a screen with your assistant.
When wearing 3D glasses I find I can still look away from the screen to look at the abdomen/ports/talk to colleagues as they act like a weak pair of sunglasses. We even find some of our anaesthetists wear 3D glasses to follow the operation (and they are still able to do their crossword!). I tend to remove my 3D glasses for skin closure at the end of the operation.
Recording video of the operation allows editing and review of the procedure to look back on technique for trainees and to submit to meetings or to show on training courses.
We use the additional CMOS camera head to perform hysteroscopy, cystoscopy and to attach to a 5 mm laparoscope to allow direct optical entry at palmer’s point. This improves the versatility of the system as it will work with pre-existing 2D endoscopes as well as with the 3D EinsteinVision scope.
We instill ICG into the bladder for laparoscopic hysterectomy after multiple caesarean sections and deeper bladder endometriosis. Unlike retrofilling the bladder with methylene blue when you only see the dye once the bladder wall is breached, ICG emits a stronger glow as the wall gets thinner during dissection. This hopefully can prevent bladder perforation before it occurs. We dilute the remaining ICG into a larger volume to adequately distend the bladder and get the dilute dye up to the uterovesical fold where the adhesion needs to be dissected free.
ICG can be injected into the uterine cavity via a uterine manipulator using the same concentration as for the ureters. During myomectomy this can help to see where the endometrial cavity is and reduce the risk of a breach. I have also used it in this way during excision of a non-communicating uterine horn to prevent a breach of the ‘normal’ horn cavity. It must be remembered that if the fallopian tubes are patent dye will pass through the tubes and into the pelvis so you should only inject small volumes to avoid the dye staining the entire pelvis and thus obscuring areas where you wish to see the dye.
ndeed, we also use ICG solution to test tubal patency instead of methylene blue at the end of surgery if we have already made up the solution (figure 4).
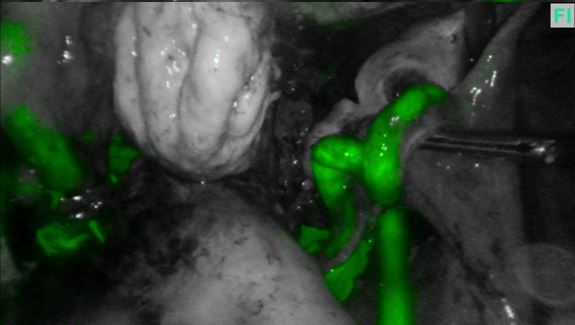
Dye test of fallopian tubes with ICG

While the cystoscopy and ureteric catheterisation can add some extra minutes to the procedure time we have found that gets quicker with experience and can be performed by gynaecologists rather than needing urology assistance.
I truly believe that the additional confidence that surrounding structures have been identified and thus not damaged helps the smooth running of the list and to get patients home more quickly after surgery.
Recording still images can help patients to understand the extent of their disease (or sometimes how healthy it is!) and to remind the surgeon or the colleagues in future as a picture can tell a thousand words.